Introduction:
Sickle cell disease (SCD) is the most prevalent inherited hemoglobinopathy in the United States. While the primary event is polymerization of HbS under deoxygenation in red cells, the contribution of white blood cells and inflammation to SCD pathology has been increasingly recognized. Prior investigations of lymphocytes in SCD revealed varied abnormalities some of which have been shown to be corrected by hydroxyruea (HU) though not uniformly (Nickel 2015, Allali 2019). Alterations in lymphocyte subsets have previously been correlated with survival in elderly populations (Ferguson 1995) and with non-AIDS related mortality in HIV (Helleberg 2014). The aim of this study was to analyze alterations of leukocyte populations in relation to different clinical outcomes in a large set of adult patients with sickle cell disease at steady state.
Methods:
Patients were consented and data was obtained as part of the INSIGHTS study (NCT02156102). Only patients with HBSS/Sβ0 from whom lymphocyte subset panels had been prospectively collected were included in this analysis. Panels consisted of total CD3+ T cells, CD4+/CD8- (CD4+) and CD8+/CD4- (CD8+) T cells, CD19+ B cells and CD16/56+ NK cells; absolute neutrophil count (ANC), white blood cell count (WBC), CD4/CD8 and ANC/ALC (absolute lymphocyte count) ratios were examined as well. Patients were classified as having cardiovascular events (CVE) if they reported prior stroke, pulmonary embolism, deep vein thrombosis, myocardial infarction, arrhythmia, cardiomyopathy, coronary artery bypass or stent. Ulcer status was defined as history of, or current active cutaneous lower extremity ulcer. Also analyzed were self-reported pulmonary hypertension (pHTN), diabetes mellitus (DM), and a combined End Organ Damage Score (EODS) consisting of one point for each of the following clinical outcomes: CVA, Any Ulcer, pHTN, CAD (MI/CABG/stent), cardiomyopathy, PE/DVT, DM. Multivariate analysis was performed controlling for age, gender and active HU use and Spearman correlation coefficients were calculated using SAS software.
Results:
170 patients were included in this analysis, 54.7% female, mean age of 38.7 years, 95.3% HbSS, 64.1% on active HU treatment, and 15.9% chronically transfused. Mean leukocyte counts were within reference ranges except for CD19+ cells (666 c/uL) which were double the upper limit of normal (ULN 321 c/uL) consistent with prior reports.
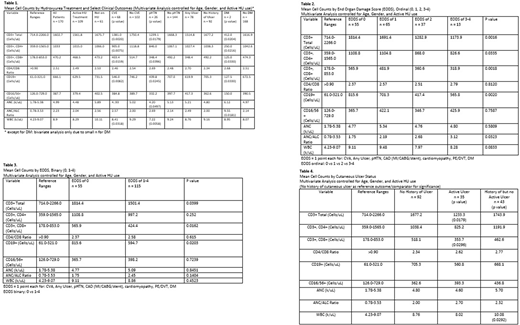
The 40% of patients with a CVE history showed an overall decrease in their lymphocyte populations (CD3+, CD4+, CD8+, CD19+) and WBC compared to those without (Table 1). Patients with a pHTN history (15.3%) had lower total CD3+, CD8+, CD19+, ANC's and WBC's. This resulted, somewhat surprisingly, in a significantly lower ANC/ALC ratio than in those patients without pHTN. No significant correlations with organ damage outcomes were noted for CD4/CD8 ratios or NK cells. Similar to the CVE findings, increased EODS was associated with significantly lower total T lymphocytes, CD4+, CD8+, and CD19+ cells while ANC/ALC ratio was significantly increased (Tables 2 & 3).
DM is very rare overall in SCD and was in our adult population (2/170) as well (Morrison 1979). It is notable that these 2 patients had significantly lower overall T and B cells and elevated ANC/ALC ratios.
Compared to patients without any history of cutaneous ulcer, those with active ulcers had significantly lower total T cells (CD3+) and CD8+ cells (Table 4) while higher total WBC was seen in patients with a history of but no active ulcer compared to those without an ulcer history.
Discussion:
Our analysis of a large cohort of adult SCD patients at steady state revealed significant alterations in leukocyte populations in relation to a variety of clinical events. The salient finding was that B and T cell lymphocyte populations were significantly decreased in relation to clinical outcomes such as CVE and pHTN. The potential impact of this finding is highlighted by the adverse survival outcomes associated with lymphopenia seen in studies of general adult populations and in those with other medical problems such as cancer (Zidar 2019, Ray-Coquard 2009). While the interpretation of this study is limited to correlations further follow-up and study of SCD immunophenotypes may reveal important prognostic information that could enhance future care strategies.
Minniti:Bluebird bio: Consultancy, Research Funding; Global Blood Therapeutics: Consultancy, Research Funding; CLS Bering: Consultancy; Roche: Consultancy, Research Funding; TauTona: Consultancy, Research Funding; Emmaus: Consultancy, Research Funding; Novartis: Consultancy, Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal